Last Updated on August 13, 2024

This episode is bought to you by Quell — to help support rebuilding healthy skin from the outside-in + inside-out!
Take $10 off your next order! Use promo code QUELL10 at check out — Get started HERE!
– – –
Did you know that a root canal could be a possible root cause for other health issues?
Or, listen on your favorite app: iTunes (Apple Podcasts) | Spotify | Stitcher | TuneIn | Subscribe on Android
My guest today is Dr. Kelly J. Blodgett, a recognized leader in holistic and integrative biological dentistry, a published researcher, author, and top clinician.
His educational background in psychology, traditional dentistry, naturopathic medical dentistry and integrative biological dental medicine provides him with a unique perspective as a healthcare provider.
He understands and respects the interconnectedness of oral health, systemic health and the feelings and emotions which accompany most people’s dental experience.
Dr. Blodgett’s professional vision is to reverse the negative stereotype associated with dentistry by sharing loving care in an environment free from judgement.
Join us as we talk about whether root canals are linked to eczema, psoriasis, or other skin conditions.
Has your root canal been linked to your skin condition? Tell me about it in the comments!
In this episode:
- Why do people get root canals?
- What can go wrong after a root canal?
- How could an infected tooth impact other tissue in the mouth?
- What to do if you've had a root canal that you suspect may be linked to other health issues you experience
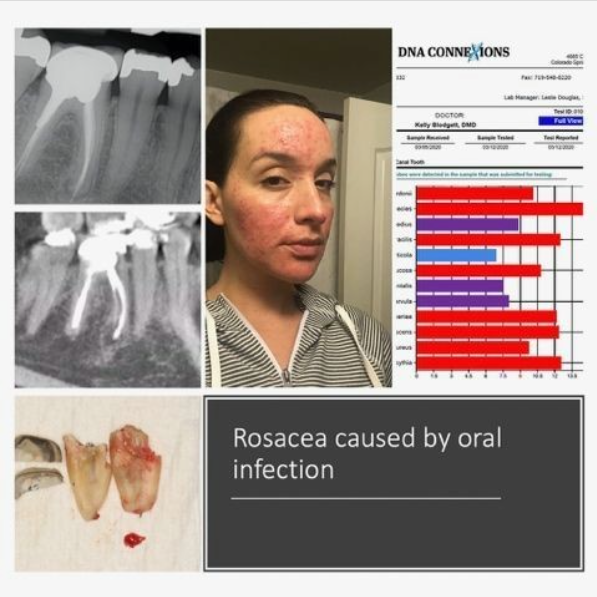
https://www.instagram.com/p/CG2X5MIAK8k/
Quotes
“Somewhere between 15 and 20 million root canals will get done in the United States this year. That's a lot of environment created that will breed infection in people's jaw bones, which is going to infect their entire health.” [8:23]
“There's this whole infectious aspect to root canal treated teeth and I've sent probably a couple of 100 teeth to a DNA lab over the last three to four years. Every single one I have sent has come back teeming with bacteria, viruses, fungi, and parasites.” [5:50]
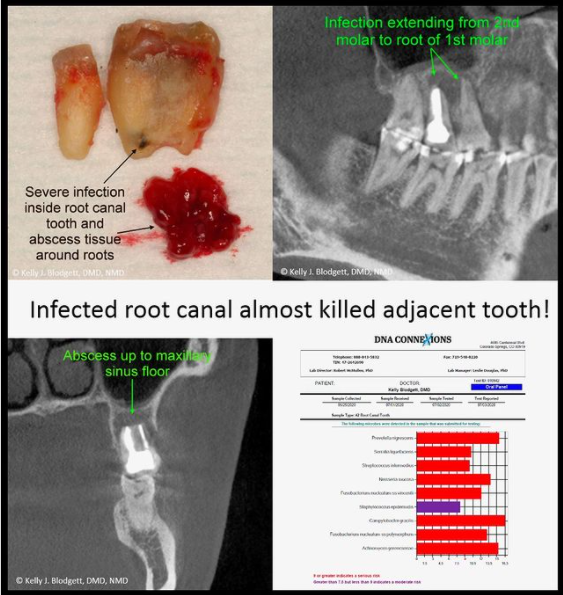
https://www.instagram.com/p/CCV-0MUARHw/
Links
How to find a holistic dentist
Follow Dr. Blodgett on Facebook | Instagram | Twitter
171: Can A Root Canal Cause Eczema, Psoriasis or Other Skin Rashes? w/ Dr. Kelly Blodgett FULL TRANSCRIPT
Jennifer: Thanks so much for joining us, Dr. Blodgett. I really appreciate you being on the show.
Dr. Blodgett: Thank you for having me. I'm thrilled to be with you today, this is awesome.
Jennifer: I am honestly probably even more thrilled than you are because, and you guys have to know this, the reason that I invited Dr. Blodgett on this podcast is because I happened to come across some very eye opening images on Instagram, and he shares some information about dentistry and how, what we're potentially doing in dentistry now, like conventional dentistry, could be part of this whole root cause system that we need to consider in the process of figuring out what is causing issues under the surface.
Jennifer: And so today, I wanted to share with you guys his thoughts and experiences, real life experiences in practice, of some of the problems that root canals can cause and I thought before that a root canal is just a root canal. Well, it's not and so Dr. Blodgett, would you help frame this conversation of like, why right now, why do people end up getting root canals and what exactly is just the basic process, especially for those of us like myself who've never had one.
Dr. Blodgett: Sure, sure. So, I mean, if I roll back to my days in dental school more than 20 years ago, I have to get into that mindset, right? The thought process is this. Let's say a tooth is either so infected that the bacteria have made their way through the hard parts of the tooth, the hard structures and into the nerve portion where you have nerves and blood flow and all that into the center of the tooth, and we call that the pulp chamber.
Dr. Blodgett: So if that gets infected or let's say somebody goes in to have some dental work done and the dentist is kind of rough with the tooth and perhaps they don't treat the tooth very kindly and it's sensitive afterwards, which is very common. Let's say they go back to the dentist and they say, “Oh geez, you did this filling and it's sensitive.” Well, then they say, “Well, it's probably super inflamed inside and you,” quote, unquote, “you need a root canal.”
Dr. Blodgett: So that's what people hear a lot. Or it could be the nerve inside the tooth simply died. Maybe it experienced some trauma, for any number of reasons. Something went wrong inside the tooth and so the dentist tells you, you need a root canal, which I could go on for probably an hour talking about the problems I have with that statement. But the process, when they do a root canal is, drill a hole into the center of the tooth, remove all of the pump material, or if it's all dissolved away because it died, they would attempt to remove whatever gunk was inside, which has usually turned to pus, and they do their best to clean out that space and dry it out and then fill that long, skinny canal system with root canal filling materials. So that's what a root canal process is about.
Jennifer: Okay. And this can go awry and there are some reasons why. And for those of you listening to this, if you, like me, need to see a photo, don't worry. I have you covered. We're going to share at least one image that Dr. Blodgett has shared on Instagram. We're going to share those within the body of this post associated with this episode because I think sometimes it's nice to talk about things, but when you really see how it shows up in real life, that can be even more shocking.
Jennifer: So what happens to that person then? So you removed this pus-y, gunky tissue, you have a root canal, and yet maybe you're having other health issues. Maybe for example, somebody is having chronic atopic dermatitis or psoriasis or some other skin issue, or it could be any other number of conditions. This is not specific to skin, this can show up in many other different ways, right?
Dr. Blodgett: Oh, absolutely.
Jennifer: So what can go wrong that you end up seeing in your practice?
Dr. Blodgett: Yeah, sure. And I think, if I may, I'll offer a little bit of the anatomy of why things go wrong first and foremost. So let's first talk about the infectious issue, right? So the problem with that whole root canal protocol is that if you're root was a solid mass that was non-porous, then the idea of a root canal could potentially work pretty well. But the problem is, is that the entire Denton material, which is like 80% of your tooth, is porous like a sponge, and bacteria, once your immune system is gone from that tooth because you've drilled out your lymphatic drainage and fresh blood supply, the bacteria have no problem climbing inside that tooth. And that was probably the biggest a-ha that I had after 15 years of extracting teeth and doing root canals was I was taking out all these teeth and you could see that the inside of the tooth had become black, but having performed many root canals, I knew that, geez, when we're finished doing the root canal, there's nothing dark inside. How does it get dark, right?
Dr. Blodgett: So there's this whole infectious aspect to root canal treated teeth and I've sent probably a couple of 100 teeth to a DNA lab over the last three to four years. Every single one I have sent has come back teeming with bacteria, viruses, fungi, and parasites. So it's not like, well, every once in a while you see some stuff in there, it's everyone that I've sent so far has been teaming with this stuff. So the infectious part is one big aspect.
Dr. Blodgett: The second issue is energetically, each tooth is connected to an energetic meridian. So I'll give you a for instance. Say your upper first molar, for instance, on both sides, happens to be connected to your thyroid gland. So you think about how many people do you talk to in your health practice who are dealing with Hashimoto's thyroiditis, something of that nature, right?
Dr. Blodgett: And the problem is people want to look at, well, let's look at your thyroid hormones and all this and that, and that's great, absolutely, that's part of the differential diagnosis. But at what point do people ask, “Have you had any dental therapy?” Because it doesn't have to be root canals, it could be energetically conducted fillings. It could be gum inflammation around those teeth. Anything that disturbs the energetic balance, right?
Dr. Blodgett: So it's both infection and energetic imbalance that can throw things off on any organ or system within the body, and nobody's asking about what's going on with people's dental health.
Jennifer: Yeah, no, it's not a question that actually any doctor I can think of has ever asked me, to be honest with you.
Dr. Blodgett: Sure, and we're not taught to, right? I mean, we're taught that if you think about it even one more step back, isn't it odd that we've got medical school and from medical school come all of your specialists like your podiatrist and your ophthalmologist and your gastrointero-, UGI health doc. I mean all of these things. But dentistry is its separate thing. It's kind of interesting, right? It's literally divorced from medicine, both from an educational standpoint and a practical functional standpoint and unfortunately, the patients are the ones who pay the price because things are being done. We're talking about root canals today, right?
Dr. Blodgett: Somewhere between 15 and 20 million root canals will get done in the United States this year. That's a lot of environment created that will breed infection in people's jaw bones, which is going to infect their entire health, and unfortunately, nobody's asking about that as they're assessing, why are they experiencing different health symptoms? And if we're not looking at it, of course it's very hard to get to the, pardon the pun, but the root cause, if we're not asking about their oral health, because it's absolutely related and connected.
Jennifer: And let's talk about that for a moment. So we've just been talking about a root canal. So when I think of that, I'm just thinking the tooth, but you just mentioned the bone, the tissue deeper than the tooth. So let's pretend here. Let's pretend I have a root canal and the tooth is loaded with black pus, all sorts of gross bacteria, fungi, et cetera. How could that then impact the tissue deeper in my mouth?
Dr. Blodgett: Yeah. So it's interesting, that tooth becomes a foreign body once it's disconnected from your blood supply and your nerves. I mean, you do have around the periphery, a ligament attachment, which slowly breaks down and the bone around that dead tooth tends to harden over time. So there are physiologic changes that occur as a result of having a dead tooth organ in your jaw bone. And of course we would expect this, right? Let's say you got a big shiv stuck in your hand or something, you would expect for those tissues to change. They'd become inflamed. You might notice some pus draining around it if you chose to leave it in there, which of course wouldn't be good.
Dr. Blodgett: But of course we should expect the gum tissue around a dead tooth to look more inflamed. We should expect the bone to start showing changes over time because it's completely dissimilar from its native state now, once it's dead. And usually what I observe, because the biggest part of my holistic dental practice now, is removing infection from people's jaws, mostly either cavitation lesions or root canals. And we tend to see bone, the initial bone around these teeth, will have a very dead quality to it and you have to remove that stuff.
Dr. Blodgett: People talk a lot about, if you read on a social media or you're doing web searches, like the idea of when a tooth comes out, do they take out the periodontal ligament, and then of course that's part of the process. But also that dense, artificially dense, what we call the laminate dura, it's this dense bone around teeth. If you don't remove that, because it's all mineralized, there's no vascular flow into that, the body is going to have a very hard time healing that.
Dr. Blodgett: So you really have to, as a clinician, we pay close attention to what is the bone telling us, so to speak, as we're cleaning that stuff out and helping their body get to a state of healing.
Jennifer: And I imagine too, having a tooth, a dead tooth, hanging out there with all of those bugs, we'll just call them bugs for the sake of this conversation, that should not be there. I try to remind people that there is a microbiome in your mouth that is different than what you have on your skin, what you have in your gut but every time you swallow, you are swallowing that microbiome, you're swallowing those bugs into your GI system and if God forbid you also have H Pylori or low stomach acid, which is incredibly common in the population that I see in my practice, people who have these chronic skin issues and it could be because of a nutrient depletion like zinc, it could be chronic stress, but H Pylori is another factor in all of this.
Jennifer: You no longer have a chemical barrier to kill these bugs and so it gives them access to your GI tract. So there's that one piece to it, but having an infected bone, is it possible that those organisms get access to your system through the blood supplier or how does that impact the body?
Dr. Blodgett: Yeah, absolutely, and this is nothing new. I find it very interesting that you look back into the 1970s even, and there's so much scientific evidence around gum disease and this acknowledgement that, well, if you've got a microbiome, essentially, periodontal microbiome that's out of balance and it's drives a person towards gum disease, that puts them at risk for, and you start just listing things off, right? Heart disease, diabetes, Alzheimer's, yada yada. So why is that not true also for dead teeth that are leaching bacteria or bugs, for simplicity, into the same cardiovascular supply chain.
Dr. Blodgett: And it's interesting because when you look at science, which I have, I've gone on Pub Med and done some Pub Med diving, there aren't any studies being done about it, which I find questionable. But given what I have seen and what I've tested myself, sending to DNA labs for analysis, I can only as a scientifically minded person come to the same conclusion that it's the same lymph drainage, it's the same cardiovascular supply that's supplying the bone around these dead teeth. Of course, that stuff is getting into your body and we should expect similar systemic effects.
Jennifer: That is a little scary to think like you just have this constant pocket of, oh goodness, an unfriendly community just hanging out kind of stewing in your system. So for people who are listening to this, because I'm imagining if I was someone who's had a root canal right now, I might be feeling a little stressed, a little freaking out at the moment. Like, “Oh my gosh, my mouth.”
Jennifer: So, all right, if you've had a root canal, does it mean that every person who's had one, I mean, I know you said every tooth that you've removed has this bacteria when you sent it off to a lab or these different organisms, do you feel that someone who has had root canals and maybe multiples should consider… What should they consider doing if they're listening to this and they're like, “Oh. My. Goodness.” What do they do?
Dr. Blodgett: Well, as I'm sure that, I would imagine we are of the same mindset, that healthcare is completely, in my opinion, it should be individualized, right? So just because Person A has a root canal on their upper right canine and Person B has a root canal on the same canine, does that mean that their bodies are going to experience the exact same scenarios of health shifts or energetic change?
Dr. Blodgett: Well, we really don't know because they're two different people, right? Their microbiomes are different. Their dietary choices are different. Their stress exposures might be different. So the impact that that one singular change might have is just going to vary from person to person. It's kind of like some people don't floss their teeth frequently and they might not even brush their teeth that frequently, yet their oral microbiome might not be horribly out of balance because of other factors in their life.
Dr. Blodgett: Maybe they eat a very healthful diet, whereas other people are fastidious about brushing, flossing, but they're drinking Diet Coke all day. You know what I mean? It's so individualized. So to answer your question, which is an excellent question, the first step would be either come and see me or find a holistic or some sort of an integrated biological dentist in your area.
Dr. Blodgett: For those who are listening to this who are Instagram followers, you can go to my May 27th post of this year, where I talk about the different avenues that you can pursue to find dentists who likely share the same sort of mindset that I'm sharing today.
Dr. Blodgett: So start there, start with a mindful dentist who's willing to listen more than they are talk because they need to hear your truth, and if they're telling you, “Well, you should do this, or you need to do that,” I would back off and go find another dentist who's asking more questions because the truth often lies in what people are sharing with us about their experience.
Dr. Blodgett: And then the second step is, and this has been something that we've brought on board in our practice more over the last couple of years, is doing different types of energetic assessments of the teeth that are in question and in this case, we're talking about root canal teeth. So let's say a person had four teeth that had had root canals and we were concerned about how those teeth are doing in their bodies. Obviously taking the tooth out and sending it out to a lab is, it's very diagnostic but it cost them the tooth.
Dr. Blodgett: So you might want to start with some sort of energetic assessment, like muscle testing, and there are a lot of different forms of muscle testing out there. EAV work, and there are also different versions of, which is known as Electro Acupuncture According to Voll. Basically using a low voltage circuit where the body and the energetic meridians of the body become the resistor in the circuit and you can actually measure energetic flow through different organs and systems and teeth, which is fascinating, and we work with some naturopathic physicians in our area who do those sorts of things for us.
Dr. Blodgett: And that has been very helpful when we're concerned because let's say a person has, they are unaware of any symptoms, right? They say, “Hey, I feel great, but I read this post and I've got three root canals and I'm concerned, is it a problem?”
Dr. Blodgett: And we might give them the information that we can, based on our dental viewing, three-dimensional x-rays, things of that nature, but energetic assessment would also be helpful. Infrared thermography might be helpful. Using the skin map and how we show heat patterns on our skin can reflect what's happening internally within our body. So we thankfully in Portland, Oregon here, we have a great thermographer that we refer to for those sorts of things.
Dr. Blodgett: So those are great, non-invasive ways to gather more quantitative information. So I would highly recommend that and if you find that somewhere in that mix of what you feel in your gut and the information that you're able to gather that you feel like, “You know what? I'm going to sleep better at night having these dead teeth out.” Well, then that's probably the right decision for you, but it's not a black and white issue by any means. We really want to gather good information, but also ask ourselves in our energetic centers, “How do I feel about this? Does this feel like it makes sense to me?”
Jennifer: Yeah, and is it the right choice, the right path forward for you.
Dr. Blodgett: Absolutely.
Jennifer: So what if someone's listening to this and they've been told they need a root canal. Would you just be like, “No”? Do you just give a straight “No,” or do you say, “It depends”? What's your opinion on that?
Dr. Blodgett: That is the one question I get on Instagram and Facebook more than any other and I do my very best to answer all those questions myself. So for those listening, if a dentist says… Let's say you present to the dentist and you have these symptoms. Usually it's my tooth hurts, right? It's either they have a cavity, my tooth hurts and I have a cavity and they say, “Well, then you need a root canal.”
Dr. Blodgett: And it's interesting because infrequently do people receive another option, right? It's just, “Well, this is what you need.” So the way that I respond to that is, “Well, it is an option.” That certainly is an option, it's one that you could choose. And the answer of whether it's appropriate for you or not depends on your individualized goals for your health.
Dr. Blodgett: If your goal is, “I want to ensure that I have no pathways for bacteria to get inside my body where it should not.” Then I would suggest you consider removing the tooth because if you do the root canal, assuredly, it will become infected. However, if your value system is such that you're not ready to remove that tooth, or let's say, God forbid, it's a teenager, either due to decay or trauma, or what have you, their skeleton hasn't completed its growth process yet and there might be some anatomical advantages to keeping that tooth for the next five years, 10 years.
Dr. Blodgett: Well then maybe in that case, the root canal would be appropriate for a period of time understanding that in the future, it would likely be best for your health to remove it. So it's really a matter of assessing a person's goals, their risk factors, where they want to be with their own personal health in their future. So it's not a quickie, “Oh, yeah, it hurts. Time for root canal.” Drilling and filling. You want a question.
Jennifer: I like the way you talk about this because I think it's important to have always the discussion of what are your health values. What is important to you? What are your goals? Because everyone's different and some people have very different feelings about what's appropriate for them and what's not. And I think that that's a really… I will say, as a person who sees dentists once or twice a year for my regular cleaning and even sees doctors, it's not very often that I've, and actually even on this show, it is not very often that any doctors and a lot of practitioners will offer this, “You should think about this in terms of your health value.”
Jennifer: So I really appreciate you actually sharing that because it's really refreshing and it's an important part of the patients, each of us, our patients, getting to have a seat at the table and be able to discuss what's really important to us for our health and ultimately make that decision so that we can be the drivers or the CEO's of what our health ultimately ends up looking like.
Jennifer: So I think this conversation is so fascinating and eye opening, and I think people are going to have questions after listening to this. I know you and I had discussed before this there's so much more to talk about, and it sounds like, everyone listening, that Dr. Blodgett will come back and will share more about a bunch of different topics involving dental health and whatnot because I do ask clients now about this in my practice. I started a number of months ago and found an alarming rate of people who had had multiple root canals and some even having redos of those root canals and they still were having issues.
Jennifer: And so this can be a long process but I think it's an important conversation that we have, so regardless of what type of issue you have, or if you know somebody in your family even, who's had root canals done, this is a great episode for them to listen to, especially if they're struggling with some sort of chronic health issue, even if it's beyond skin.
Jennifer: So I just want to thank you so much, Dr. Blodgett. This was amazing. You blew my mind. Totally blew my mind.
Dr. Blodgett: Well, thank you for bringing this to light because it will be through the awakening and creation of awareness of the public at large, that things that are being done to them, which frequently they feel like they have no choice over, if we don't create awareness, no change will ever happen. So I applaud you for bringing this out and I am so grateful to be a part of sharing it with you. So thank you very much for asking me, I'd absolutely love to come back.
Jennifer: Yes, and so for anybody who's curious to connect with you, so first of all, you're out in Portland, Oregon, correct?
Dr. Blodgett: Portland, Oregon. Beautiful Portland.
Jennifer: Beautiful Portland, and you can find Dr. Blodgett at blodgettdentalcare.com. He's also got two separate Instagram handles, we'll put both of those on his website and his Facebook page link over on… I'm going to redo that for who's editing this.
Dr. Blodgett: And if you want to, just tell them just the @blodgettdentalcare is fine because I don't look up anything else.
Jennifer: Fair enough. Fair enough. So you can go on over to blodgettdentalcare.com, and he's also on Instagram @blodgettdentalcare, and we've got Facebook and Twitter links as well that we'll share. We'll put everything on the show notes for you guys, so it's really easy for you to connect with Dr. Blodgett and his team, especially if you're looking for more information. He's got a ton and it's very, very informative. It's easy to understand. It's very eyeopening and at the least, if you're not able to travel to Portland, you might be able to start asking better questions of your dentist during your routine care visits, as well as if you're starting to have issues.
Jennifer: I think this is an important conversation to be had, and I just deeply appreciate you, Dr. Blodgett, for sharing this information with us.
Dr. Blodgett: Well, thank you so much for having me. I really appreciate it.

Jennifer Fugo, MS, CNS
Jennifer Fugo, MS, CNS is an integrative Clinical Nutritionist and the founder of Skinterrupt. She works with adults who are ready to stop chronic gut and skin rash issues by discovering their unique root cause combo and take custom actions with Jennifer's support to get clear skin (and their life) back.






This was so timely for me. I was told to get my root canals out. I said absolutely not. I would like to know options for after tooth is pulled. I opted to have a tooth pulled last year instead of another root canal. I was told I was crazy to do that. I see a holistic dentist, he’s the one who removed my amalgam fillings, and pulled my tooth. Do not trust him enough to do anymore of my work outside of cleaning. I’d love to know options for having root canals removed then what??
This is such an excellent interview. I found it researching the root canal connection with diseases. Reason being, I know for sure, since I’m 73, know my body, and have been researching health and disease for YEARS. Loving the internet. As a kid I had bad teeth and had root canals, bridges, mercury fillings, etc. One year I started focusing on the tooth/organ connection from what I learned from info on Dr Weston Price. Well, now I know there is a connection to EVERYTHING. Moved and was searching biological dentists but one day my one tooth (#3) which on the tooth/organ chart indicates so many things, was hanging off. so I had to go local. he pulled it, drilled into the bone to do a tooth implant. I didn’t want to take antibiotics, but actually probably should have. I did have major swelling, and lethargy, but nothing else. I eat all organic and a health researcher. So one day I called the dental office and asked if by any chance that tooth was next to the one with the root canal. she said, um. it WAS that tooth. I’m like, crap. I got the number of the tooth wrong from my previous dentist. in any case. I have now a few serious lesions on my skin (upper thigh same side) I know I never had this before. But even before that, after waiting months after the first segment of the implant (the final phase was due months before, but I wanted to be sure all was healed before they opened that area again) I decided to go get the cleaning and x-rays on my deal with them. well then that’s when all hell broke loose. my nose had sudden open, bleeding sores, my face on that side got big dark lesions, and more. As I mentioned I’m 73, but on no meds, perfect vision, (used to wear glasses but another story) don’t have a medical doctor, virtually no grey hair (oh yeah that’s another thing. all of a sudden I now have 50% grey hair, esp on same side as tooth) walk 3 miles most days… pretty good. needless to say I am now going to go find a biological dentist and drive hours if I have to.